(C) 2024 Renewed | Vernon R. Stanley, MD PhD. All rights reserved.
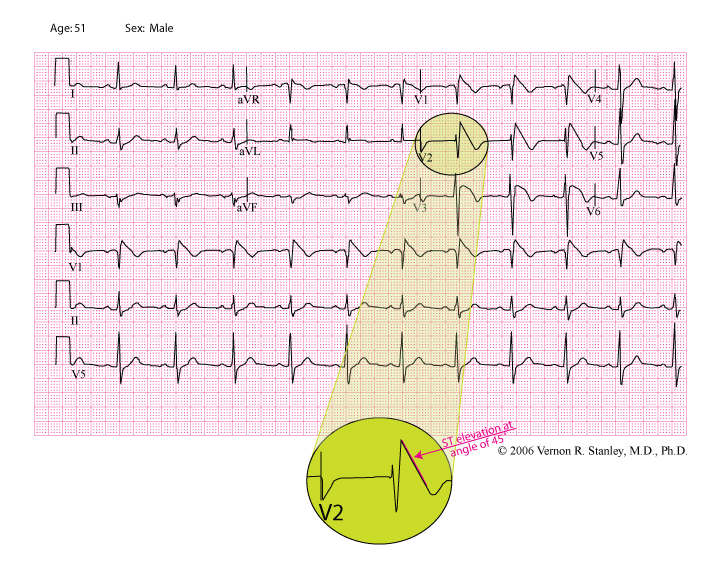
This case study is a classic example of the Brugada Syndrome on the 12-lead ECG. You can easily see from the tracing below why one might interpret the tracing as one of an acute ST-elevation MI or STEMI (Anteroseptal). Note particularly the ST elevation and T-wave inversion in Lead V3.
Brugada Syndrome is a cardiac abnormality and genetic disorder (autosomal dominant transmission). It is characterized by an electrical abnormality with a structurally normal heart. The syndrome proper is characterized as follows (without symptoms it is referred to as the Brugada Sign):
- Clinical episodes of near syncope, syncopal episodes, seizures or sudden death.
- Structurally normal heart.
- Characteristic ECG pattern displaying ST elevation and T-wave inversion/biphasic T’s in Leads V1, V2 and V3 (pattern resembles RBBB).
Incidence of Brugada Syndrome
This syndrome has been recognized virtually worldwide, less common in the United States and most common in southeast Asia (Thailand and Laos). It is stated to be responsible for five deaths per year per 10,000 population in areas where it is endemic. The arrhythmia leading to sudden death is Polymorphic Ventricular Tachycardia
(Torsades de Pointes) with degeneration to ventricular fibrillation.
12-lead ECG Characteristic of the Brugada Syndrome
For emphasis, I have magnified Lead V2. Please note that the ST-segment has been labeled and color-coded pink. The ST segment assumes a peculiar ramp-like elevation at an angle of nearly 45 degrees. The T-wave is inverted (negative). These ST-T changes are the hallmark of the Brugada Syndrome.
Common misdiagnosis of the Brugada Tracing
A careful analysis of the tracing above will reveal why Brugada Syndrome is frequently misdiagnosed as the following:
A. Atypical RBBB – This tracing demonstrates RSR’ in Lead V2 with a biphasic Lead I and small terminal S-wave. The QRS duration is slightly prolonged.
B. Acute Anteroseptal MI, with ST elevation (concave down) in Leads V1, V2 and V3 and T-wave inversion or biphasic T-waves in Leads V1, V2, and V3.
Treatment
If treatment is indicated, please know that the objective would be directed to the prevention of Ventricular Tachycardia and sudden death. Some patients with electrocardiographic changes of Brugada Sign might be negative for sudden death and the patient’s history might be negative for syncope, pre-syncope or seizures. However, ALL patients you encounter in your practice with these classic ECG findings should be referred to the cardiologist for a work-up and treatment recommendation (choose a cardiologist who has a familiarity with this disorder).
If the patient is experiencing symptoms related to transient Ventricular Tachycardia, antiarrhythmic drugs including beta blockers and amiodarone, are ineffective to prevent Ventricular Tachycardia and sudden death. The only effective treatment mode is the automatic implantable defibrillator.
Additional information regarding the Brugada Syndrome
- Brugada is characterized by ST-segment elevation in Leads V1, V2, V3 with a peculiar slant at approximately 45 degrees and T-wave inversion or biphasic T-waves.
- The disorder occurs worldwide but is most common in Southeast Asia.
- The QT interval is usually normal.
- The only treatment to avoid Ventricular Tachycardia, Ventricular Fibrillation and sudden death is the automatic implantable defibrillator.
- Incidence of the Brugada Syndrome male:female is approximately 8:1.
- Death commonly occurs during rest or sleep (in Thailand, it is known as “lai tai” [“death during sleep”]).
- It is a genetic disorder.
- Medications such as Amiodarone or beta blockers do NOT prevent sudden death.
- With no known history of cardiac disease, Brugada is the most common cause of sudden death age < 50 years in South Asia.
- This disorder may be the leading cause of natural death among young men in poverty-stricken Northeast Thailand.
STRENGTHEN YOUR KNOWLEDGE OF 12-LEAD ECG Interpretation.
Register for the Comprehensive 12-lead ECG Course (30 hrs Cat I CME/CE) or the 50 Case Study Review Course (13 hours Cat I CME/CE).
©2024 Renewed Vernon R. Stanley, MD, PhD. All rights reserved.